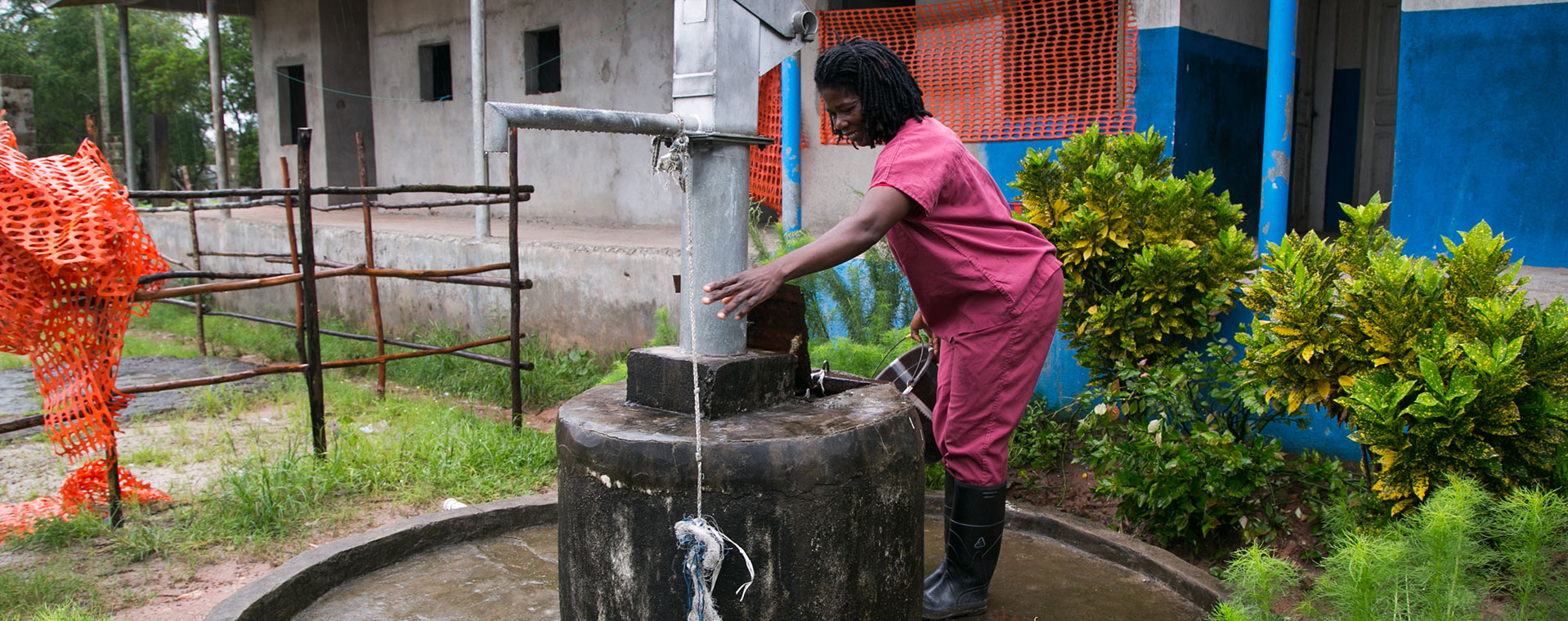
I spent my first days in the NICU; I got lucky
STORIES |
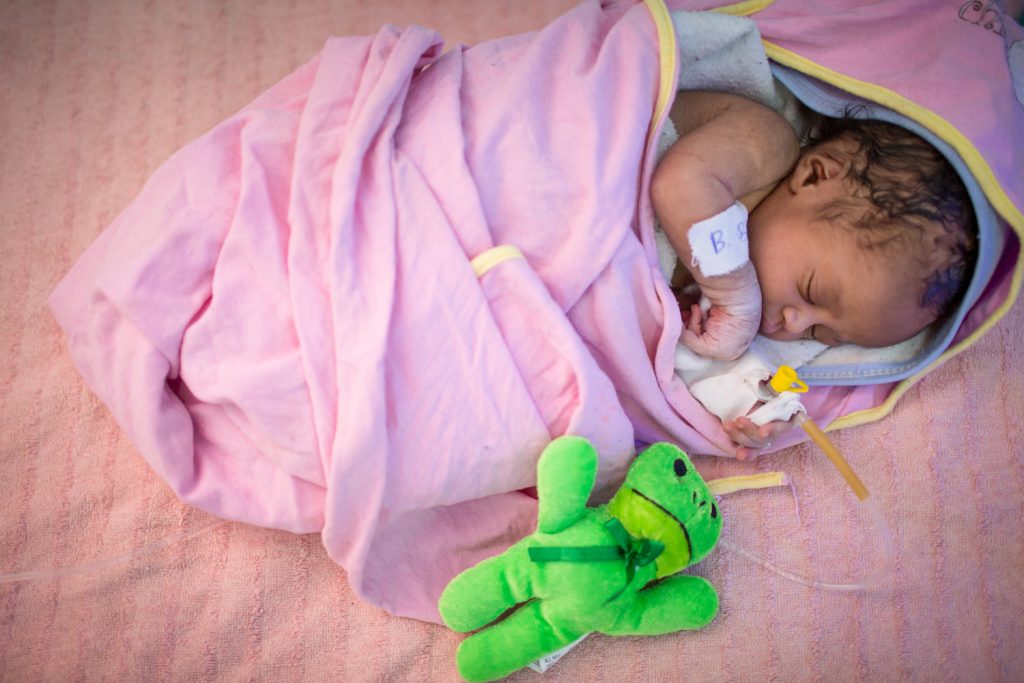
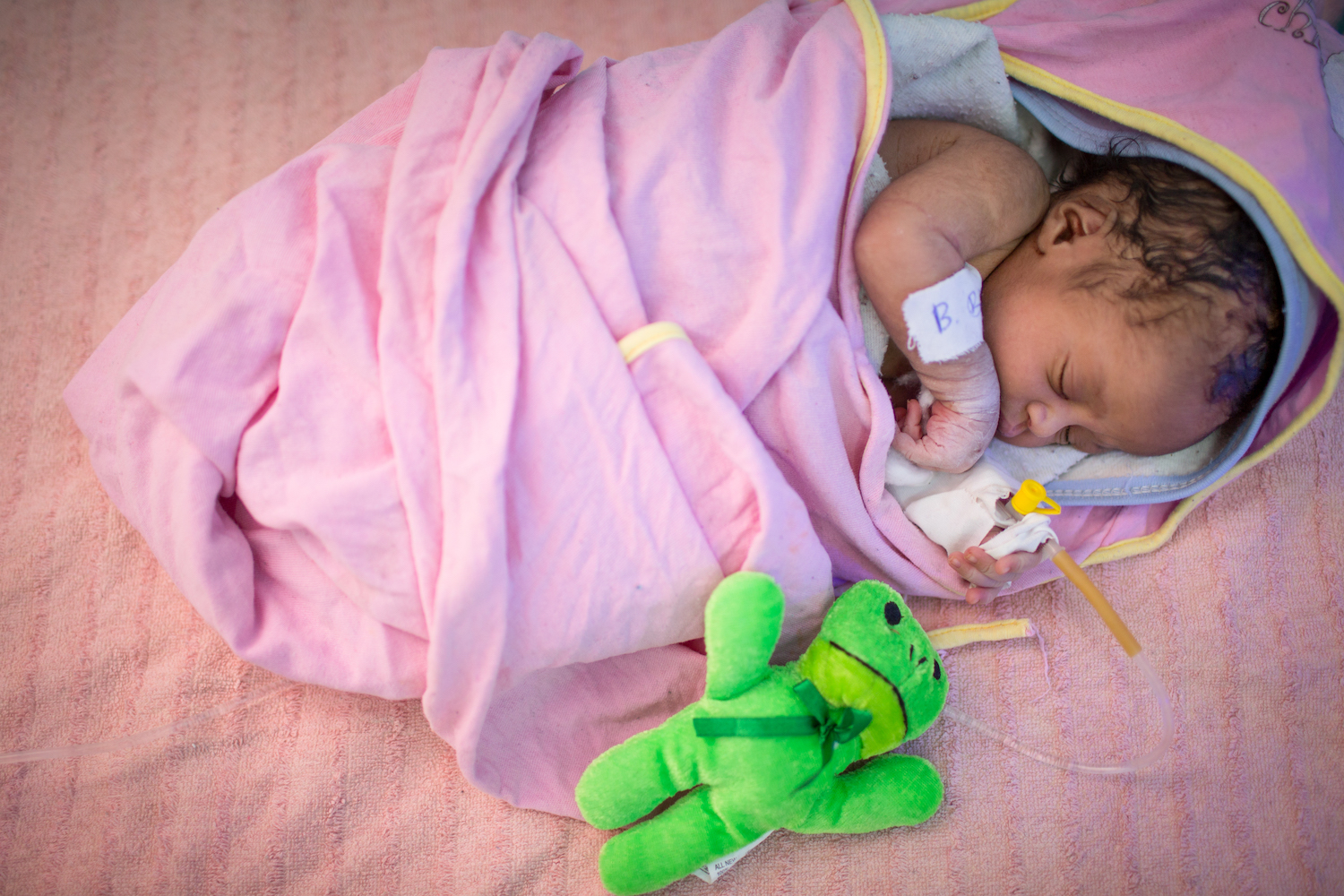
©UNICEF/UN0220402/Ayene
A newborn infant receives specialised care at the UNICEF-supported Neonatal Intensive Care Unit (NICU) at Assosa General Hospital, in a remote region of Ethiopia.
An intern on duty told me it was not uncommon for a baby to contract an infection, which then rapidly spreads to the others. Ethiopia is by no means alone. Health care-associated infections in fragile newborns are three to 20 times higher in resource-limited settings compared to more high-income contexts. In some cultures, newborns are not named their first week because mortality rates are so high.
The ongoing lack of hand washing facilities is especially troubling and well-documented in data just released by UNICEF and WHO. They found that 1 in every 3 health care facilities does not have water, soap or hand sanitizer where patients receive care; yet we know hand hygiene is the most effective defense against dozens of illnesses and diseases, with COVID-19 now topping the list. When handwashing and clean birthing practices are in place in the health care setting, newborn survival rates increase up to 44%. The health benefits continue through the first five years of life. Common diseases, like diarrhoea, take over 400,000 lives under age five every year. Simply handwashing with soap can reduce diarrheal episodes by 45%.
Instead, women in low-resource settings must give birth in health care facilities without adequate water, sanitation and hygiene (WASH). Around the world, women in labour must haul their own water, of questionable quality, to give birth in health care facilities that cannot be adequately cleaned. Umbilical cords are cut with dirty instruments on tables wiped down with dirty rags. Making it more likely that some of those newborns will end up in a NICU (if available), or die preventable deaths.
Still, babies continue to be born. Diseases require medical interventions. Accidents must be treated. And health care workers continue to provide care every day in the face of a historic pandemic. The doctors, nurses, midwives and cleaners in these poorly equipped facilities put themselves and their patients at risk every day, because they can’t adequately wash their hands. In these settings, soap and water may be the primary — or only — PPE and too many doctors, nurses, midwives and cleaners don’t have either.

© Tom Greenwood/WaterAid
WHO recommends a “multi modal strategy” for hand hygiene in health care facilities to establish “clean safe care” through a culture of hygiene among all staff.
The nearly two billion people who must rely on health care facilities that lack basic water service, and the staff who work there, need and deserve a safe and dignified health care environment. It’s a complex challenge that will require a multi-pronged solution. Training on hand hygiene in health care facilities that lack soap and water does little to support behaviour change. But the availability of soap and water does not automatically lead to improved handwashing behaviors, so installing new sinks without addressing prevailing attitudes and habits is unlikely to make a marked improvement. A third consideration, designing infrastructure and behaviour interventions without accountability and monitoring from the health care facility on up to the Ministry of Health will result in costly unsustainability … broken pipes, sinks, faucets and dirty hands. WHO recommends a “multi modal strategy” for hand hygiene in health care facilities to establish “clean safe care” through a culture of hygiene among all staff. This approach includes proper WASH resources, and training on handwashing, and supervision, coaching, and job aides. The comprehensive approach, the report notes, has proven highly effective at improving handwashing practices and reducing infection rates.
COVID-19 has certainly underscored the need for a consistent supply of clean water in health care facilities and could provide a model for hygiene elsewhere, like in homes and schools, where access to water is again a core health issue. Three billion people (40 per cent of the world’s population) can’t wash their hands at home, putting an estimated 1 billion people at immediate risk of COVID-19. As kids head back to school, 2 in 5 schools do not have handwashing facilities — that’s 818 million children.
This new UNICEF/WHO report tells us that we are making progress, and together countries and partners are stepping up the challenge. But there is much more to be done — in particular broadening planning, financing, and monitoring of WASH services — to ensure health care facilities everywhere have sustainable access to safe water, clean toilets, and soap. If we really do achieve a culture of hand hygiene with access to sustainable WASH, the illnesses and diseases prevented would save untold unnecessary suffering and death. UNICEF and WHO rightly describe WASH as “non-negotiable” in the health care setting. As someone lucky enough to have been cared for in a clean and safe NICU, I couldn’t agree more.
Lindsay Denny, a senior public health program associate for the Center for Global Safe Water, Sanitation and Hygiene at Emory University, is the health adviser for Global Water 2020.
This article was originally posted on UNICEF Connect